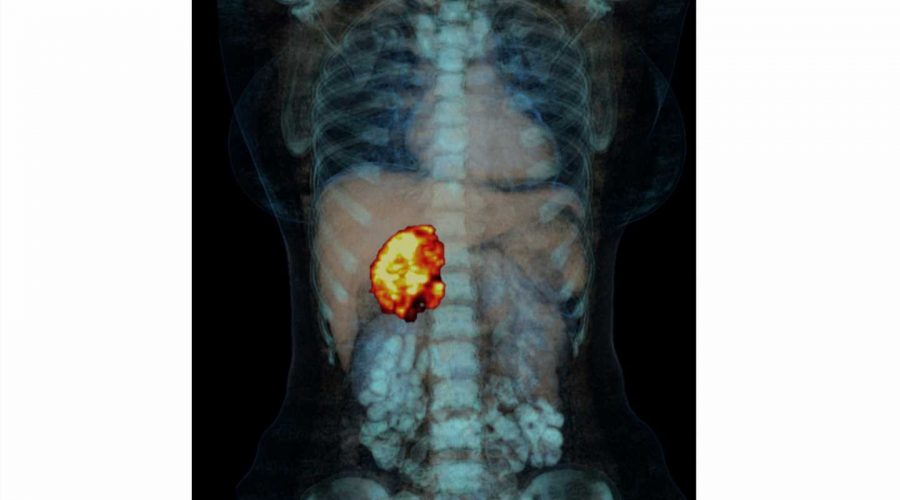
Study shows no mitotane needed for patients with low risk of recurrence of adrenocortical carcinoma
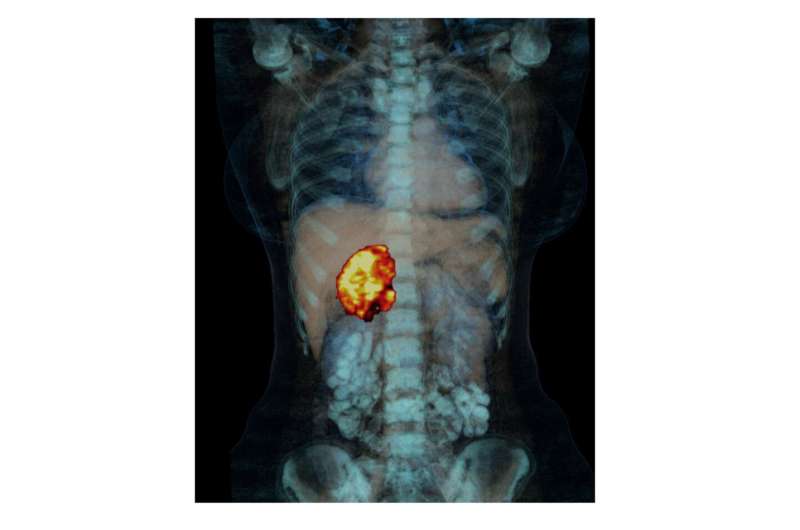
In 2007, the teams of Massimo Terzolo and Martin Fassnacht published a study in the New England Journal of Medicine that provided evidence for the efficacy of mitotane in the prevention of recurrence in adrenocortical carcinoma. This study established the drug worldwide as a standard therapy for relapse prophylaxis after surgical removal of the tumor, regardless of risk factors that were still unknown at the time.
Mitotane inhibits cell division in the adrenal cortex and thus counteracts tumor growth. The risk of the disease coming back after surgery was three times higher in the control study group that did not receive mitotane than in the mitotane group. And the risk of dying from the disease was almost halved by the therapy. The Italia-German team had set new standards in the treatment of the very rare but extremely aggressive tumor.
“Our findings from 2007 still apply, but only to patients with normal or high risk of recurrence,” explains Prof. Dr. Fassnacht, chair of the Department of Endocrinology and Diabetology at Würzburg University Hospital.
In a new clinical study published in August 2023 in the journal The Lancet Diabetes & Endocrinology, he and Terzolo and other collaborators found that the adjuvant treatment with mitotane is not necessary if the patients fulfill three factors. First: The operation was a complete, so-called R0 resection. Second: The tumor stage was low and there had not yet been any spread. Third: The cell proliferation marker Ki-67 is below 10%, meaning the risk of recurrence is low.
ADIUVO shows no improvement with low risk of recurrence
ADIUVO is the first ever randomized trial worldwide of adjuvant treatment for adrenocortical carcinoma. A total of 91 patients in 23 centers in seven countries were randomized to either receive oral mitotane for two years or to be monitored “only” by imaging and laboratory controls after surgical removal of their adrenocortical carcinoma and low to intermediate risk of recurrence (R0 resection, stage I-III, Ki67 ≤10%). The efficacy of mitotane versus surveillance only was assessed by recurrence-free survival (RFS).
The 5-year RFS rate was 79% in the mitotane group and 75% in the surveillance group. The 5-year overall survival rate was not statistically significantly different. However, all study participants who received mitotane experienced adverse events, and eight people discontinued treatment. Mitotane treatment can be associated with nausea, diarrhea, dizziness and even speech problems. Patients who did not want to be randomized were followed up in a prospective follow-up study. These were 95 people, of whom 42 were followed up with mitotane and 53 without. In this parallel study, the result of the randomized study was confirmed.
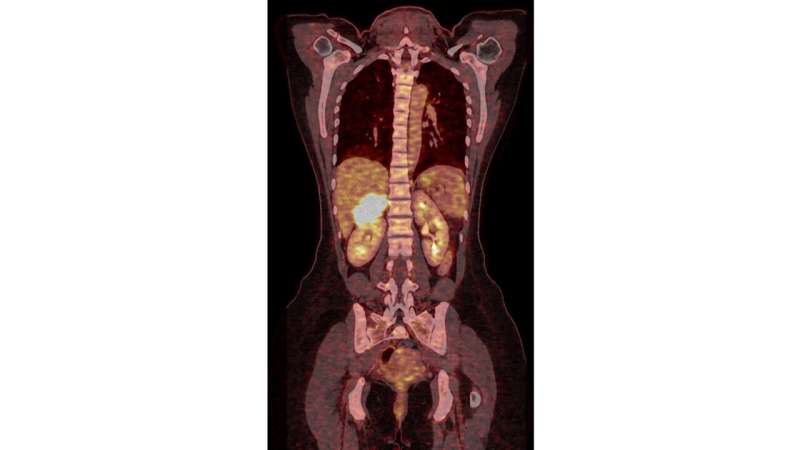
Prognosis scheme based on tumor stage, resection status and Ki-67 assessment
Fassnacht states, “Concomitant therapy with mitotane is not indicated in patients with low-grade, localized adrenocortical carcinoma in which the tumor has not yet metastasized and could be completely removed, as their prognoses are relatively good and treatment with mitotane does not show a statistically significant improvement in the relapse rate, but is associated with side effects.”
In other words, “our study is a first step towards personalized medicine in this rare disease. It shows that it is possible, with a simple and widely available prognostic scheme based on tumor stage, resection status and Ki-67 assessment, to identify a subgroup of patients whose prognosis is much better than expected and for whom active surveillance is the most appropriate approach.”
Endocrinology at Würzburg University Hospital is considered an international reference center for the diagnosis, treatment and research of adrenocortical carcinoma and is currently the largest center worldwide. The usually highly malignant tumor of this endocrine gland, which sit in pairs on the kidneys, has been the focus of Würzburg endocrinology for more than 20 years.
The European Adrenal Tumor Network ENSAT and the German Adrenal Carcinoma Study Group are coordinated from here. “With our numerous basic research, translational and clinical studies, we in Würzburg, together with a large interdisciplinary team, have made a significant contribution to improving the worldwide diagnosis and treatment of patients with adrenal carcinoma,” Fassnacht says.
Even the diagnosis is difficult, because adrenal carcinoma is very rare and initially causes no symptoms. Therefore, it is often only discovered at an advanced stage. In Germany, it is estimated that there are about 80 to 120 new cases every year. Depending on the type of tumor, surgery can be performed, and in the advanced stage, chemotherapy or radiotherapy are also necessary.
Until now, it was common practice to treat all patients with additional medication after surgery, regardless of the stage of the tumor. Currently, mitotane is the only approved drug for adrenal carcinoma. Clinical studies on other drugs and therapies are underway at the University Hospital of Würzburg.
More information:
Massimo Terzolo et al, Adjuvant mitotane versus surveillance in low-grade, localised adrenocortical carcinoma (ADIUVO): an international, multicentre, open-label, randomised, phase 3 trial and observational study, The Lancet Diabetes & Endocrinology (2023). DOI: 10.1016/S2213-8587(23)00193-6
Journal information:
New England Journal of Medicine
,
The Lancet Diabetes & Endocrinology
Source: Read Full Article