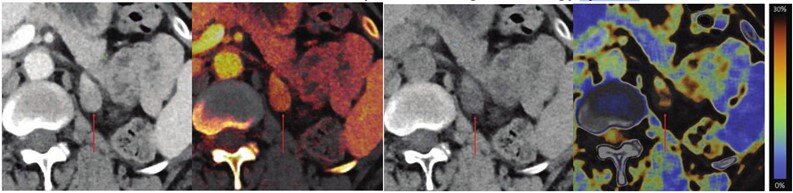
Dual-energy CT metrics for differentiating adrenal adenomas
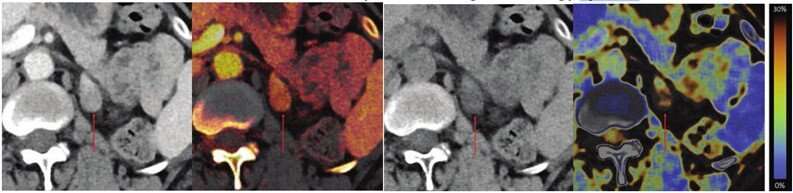
According to a study published in the American Journal of Roentgenology (AJR), for adrenal lesions evaluated by single-phase dual-energy CT (DECT), fat fraction had higher sensitivity than virtual noncontrast attenuation at both the clinically optimal threshold and at the traditional ≤10 HU threshold.
“DECT-based three-material decomposition algorithms can help definitively characterize adrenal lesions detected on routine abdominal imaging as adenomas, thereby reducing downstream follow-up testing,” wrote first author Anne-Sophie T. Loonis, MD from Brigham and Women’s Hospital in Boston, MA.
In this AJR accepted manuscript, 128 patients (82 women, 46 men; mean age, 64 years) who underwent portal-venous phase abdominopelvic CT between January 2016 and December 2019 showed a total of 139 adrenal lesions with a reference standard based on imaging, clinical, and pathologic records: 87 adenomas, 52 nonadenomas (48 metastases, 2 adrenal cortical carcinomas, 1 ganglioneuroma, 1 hematoma).
Two radiologists located ROIs to determine virtual noncontrast attenuation, fat fraction, iodine density normalized to portal vein, and relative enhancement ratio—for masses with virtual noncontrast attenuation >10 HU.
Ultimately, for adrenal masses assessed by single-phase portal-venous phase DECT, when maintaining 100% specificity, sensitivity for adenoma was significantly higher for fat fraction [59% (95% CI: 48-69%)] than for virtual noncontrast attenuation at clinically optimal threshold [39% (95% CI: 29-50%)] or at traditional ≤10 HU threshold [28% (95% CI:19-38%)].
“The use of DECT-derived metrics to definitively diagnose incidental adrenal lesions as adenomas could help avoid the costs, radiation exposure, contrast media exposure, and patient anxiety associated with downstream imaging that may otherwise be performed for further lesion characterization,” the authors clarified.
More information:
Anne-Sophie T. Loonis et al, Dual Energy–Derived Metrics for Differentiating Adrenal Adenomas From Nonadenomas on Single-Phase Contrast-Enhanced CT, American Journal of Roentgenology (2022). DOI: 10.2214/AJR.22.28323
Journal information:
American Journal of Roentgenology
Source: Read Full Article