Antibiotic overprescribing permeates US hospital ICUs, finds study
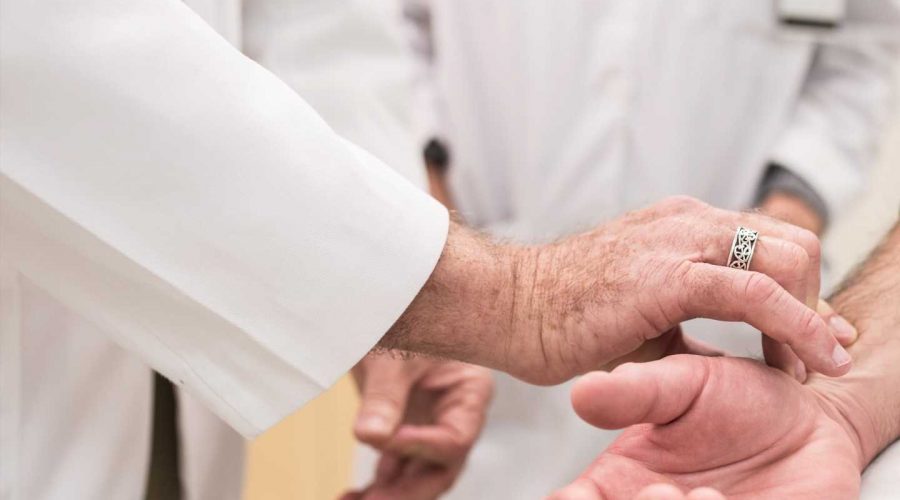
In the United States, physicians in almost every specialty and role use antibiotics as part of their therapeutic armamentariums. Antibiotic prescribing is a longstanding part of medical practice for hospital-based physicians.
Medical intensive care units (ICU) are battlegrounds of antimicrobial resistance; ill patients get admitted for hospital stays, during which most are given antibiotics. During the rush to provide care, many of the interventions put in place have been critically analyzed as potentially “excessive and inappropriate.” For example, up to 70 percent of ICU patients receive antibiotic therapy on any given day, and 30 to 60 percent of those antibiotic prescriptions are unnecessary.
A study by a Florida Atlantic University researcher and collaborators examined how ICU physicians in both a public and a private hospital utilized antibiotic therapies and what factors influenced their antibiotic decision-making.
Researchers explored how physicians communicate about, decide upon, and document antibiotic prescriptions as well as how they engage with the expectations and guidelines such as those related to antimicrobial stewardship, a leading form of intervention aimed at improving antibiotic prescribing and a recent requirement for U.S.-based hospital settings.
The study was conducted in 2018, prior to the COVID-19 pandemic, and study participants were all specialists in pulmonary and critical care, divided across a range of rank and seniority.
Results, published in the journal Social Science & Medicine, reveal that there continues to be an “antibiotic culture,” meaning that the preference for antibiotics is related to their perceived role as “magic bullets.” Findings showed a context-specific culture of antibiotic prescribing most closely associated with the patient load and ICU processes.
Antibiotic prescribing was shaped by urgency, hierarchy and uncertainty. Existing ICU workflows and the pressure to treat patients in an urgent manner, especially those with complicated cases, led to increased antibiotic use. Study participants also recognized an interconnectedness with other teams working in the unit and used timeliness as a rationale for antibiotic prescribing.
“By studying the culture of antibiotic prescribing in ICUs, we can see more clearly both the vulnerability of the looming antimicrobial resistance crisis and by contrast the perceived insignificance of stewarding antibiotic use when considered alongside the fragility of life amidst acute medical concerns regularly experienced in the unit,” said Katharina Rynkiewich, Ph.D., senior author and an assistant professor in the Department of Anthropology within FAU’s Dorothy F. Schmidt College of Arts and Letters.
Rynkiewich conducted the research as a Ph.D. student at Washington University and later completed the project as a postdoctoral scholar at Case Western Reserve University. As an anthropologist of health and medicine, she is continuing her research on the social and cultural dynamics of U.S. antibiotic prescribing practices at FAU.
Overall, findings showed the continuing pattern that urgency and timeliness were prioritized over continued mindful discussion of antibiotic selection, dosing, duration, and the various other considerations that come into play with antimicrobial stewardship. Ultimately, the lack of sustained, mindful discussion surrounding antibiotic selection contributed to uncertainty about antibiotic use during critical moments of urgency in the unit.
“Our study results relate antibiotic prescribing in the ICU to preexisting conditions of the setting: time pressures and urgency, dependence on other teams, and uncertainty resulting from providing care for patients with complex, severe illnesses of uncertain cause(s) at the time of presentation,” said Rynkiewich. “The interviews we conducted illustrate that physicians have learned the ways antibiotics fit within their day-to-day practice and how their decision-making is prioritized differently from other teams such as pharmacy.”
Researchers found the context of the ICU and the social dynamics of those present in the setting created a uniquely strained culture of antibiotic prescribing. It was clear from the respondent interviews that once an antibiotic had been decided upon, there was an urgency to have it administered to the patient. This concern was not just reflecting a desire for the unit to be efficient, but a frustration about the lost time that could negatively impact a patient’s recovery.
“While the ICU is a setting where many critically ill patients are admitted, and those patients are at risk of having an infection, selective and judicious antibiotic prescribing finds a negotiated place among other priorities such as stabilizing the patient followed by working towards a plan of discharge,” said Rynkiewich. “For us, detailing how antibiotic prescription is a complex and dynamic social process in acute care hospital spaces adds value by unveiling the otherwise unwieldy black box of ‘culture.'”
As global challenges such as antimicrobial resistance and viral pandemics become intertwined in their broad impact, the researchers say that conduct of social science research aimed at uncovering diverse and manifold contexts of antibiotic use only grows in its significance.
“The future of antibiotic-resistant pathogens is driven, in part, by how society decides to utilize antibiotics. These decisions are influenced by changing environmental conditions such as was experienced during the COVID-19 pandemic when estimates show that nearly 70 percent of patients with suspected cases of COVID-19 received antimicrobials,” said Rynkiewich. “Furthermore, antimicrobial stewardship in settings such as ICUs became deprioritized while attention shifted to the pandemic.”
More information:
Katharina Rynkiewich et al, Cultures of antibiotic prescribing in medical intensive care, Social Science & Medicine (2023). DOI: 10.1016/j.socscimed.2023.115834
Journal information:
Social Science & Medicine
Source: Read Full Article